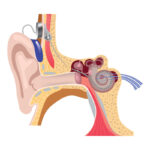
If you're considering the possibility of developing sensorineural deafness, you should know the symptoms, causes, and treatments of the condition. Listed below are some of the more common symptoms, causes, and treatments of this condition. Listed below are the most common nonsyndromic causes of sensorineural deafness. Detailed information on each of these causes can help you choose the appropriate treatment.
Symptoms

Sensorineural deafness is a disorder of the inner ear that causes hearing loss. This condition is caused by damage to the auditory nerve, inner ear, and brain. The symptoms of sensorineural deafness are not as severe as other types of hearing loss, but they can still be bothersome. Early diagnosis is critical to successful treatment. However, delaying treatment may lead to worse hearing loss.
People with sensorineural deafness may experience problems hearing at any range, but most sufferers experience a high-frequency loss. This means that they have a difficult time understanding speech, especially when it is surrounded by background noise. Hearing aids can help improve these problems, but they must be programmed to correct the individual's hearing loss. Proper fitting is essential. To treat sensorineural deafness, you should schedule an appointment with a hearing healthcare professional immediately.
In some cases, sensorineural deafness may develop suddenly. This condition can be caused by exposure to loud noise, illness, certain drugs, or a hereditary condition. In most cases, hearing aids are beneficial. However, sudden sensorineural deafness that lasts for days or weeks should be treated immediately. Delaying treatment may decrease the effectiveness of the medication. However, there are many treatments for sensorineural deafness.
Causes
Some of the most common causes of sensorineural deafness are hereditary, i.e., hereditary, and genetic. Some of these types of deafness are caused by mutations in the genes KVLT1 and PDS, which are found in both sexes. Other causes of sensorineural deafness are caused by birth defects or heredity.
The sixth disorder, which causes permanent sensorineural deafness, is caused by a lack of an enzyme in the pancreas. This condition affects one in every 25,000 live births. It affects both sexes equally and is hereditary in one or both parents. It can cause malabsorption and lead to hearing loss. It is usually inherited from one parent, although the condition can also be acquired from a family member.
In addition to hereditary hearing loss, other causes of sensorineural deafness include repeated exposure to loud noises, treatment with certain antibiotics, tumors, and skull fracture. Some premature infants have sensorineural deafness because of their abnormally short gestation period. While the most common reason is prolonged exposure to loud noises, other causes are infection in the back of the nose or throat.
Treatments

Sensorineural hearing loss occurs when damage to the inner ear, specifically the auditory nerve, prevents the sound from being transmitted to the brain. These conditions can be caused by head trauma, exposure to loud noise, or ototoxic drugs. The sooner this condition is diagnosed and treated, the better. Treatment for sensorineural deafness may be insufficient for severe cases, but can slow down the deterioration of hearing.
There are many treatments available for sensorineural hearing loss. In some cases, the condition may be induced by an allergic reaction to a particular drug. Surgical procedures and ototoxic medications are commonly used. Sudden sensorineural deafness is often treated with a tapered course of high-dose corticosteroids. Other treatments include hyperbaric oxygenation. However, these treatments are not indicated for most cases of sensorineural deafness.
Although there is no cure for sensorineural deafness, it is treatable and may even be curable. A professional audiologist can assess a patient's hearing health and recommend a hearing aid or cochlear implant. Cochlear implants can be used in severely deafened individuals. In rare cases, a cochlear implant may be the best treatment.
Nonsyndromic causes
There are two types of hearing loss: syndromic and nonsyndromic. Syndromic deafness involves other parts of the body. Nonsyndromic deafness involves changes to the inner ear. Autosomal dominant deafness results from an altered gene inherited from one parent who suffers from the hearing loss. Fortunately, nonsyndromic deafness is rare.
The most common nonsyndromic causes of sensorineural hearing loss are genetic. Approximately one out of every 1,000 live births has some form of deafness. Around 80% of genetic causes are autosomal recessive. Genetic causes are primarily caused by mutations in the connexin26 gene. This gene is involved in language development and is responsible for causing hearing loss.
Nonsyndromic deafness is caused by the presence of a mutated gene on the X chromosome. Males with this mutation typically develop severe hearing loss at a young age. In contrast, fathers do not pass the X chromosome to their sons. Another type of nonsyndromic cause of sensorineural deafness is caused by changes in the mitochondrial DNA. This gene is inherited from the mother and is not passed on from father to son.
Meniere's disease
Symptoms of Meniere's disease often include dizziness, tinnitus, and a fullness sensation in the ears, similar to the sensation of varying altitude. Despite the presence of other symptoms, it is difficult to diagnose Meniere's disease without objective diagnostic testing. Electrocochleography and glycerol dehydration tests are the main diagnostic tools for this disease.
Vertigo is the most common symptom of the condition. Attacks usually begin suddenly and may be accompanied by nausea or vomiting. The average vertigo spell lasts for several hours. Patients experience fatigue even after the vertigo has subsided. Vertigo spells may come and go and can be unpredictable, especially if the disease is idiopathic. Hearing loss generally affects only one ear but can be severe.
The ideal surgical treatment for Meniere's disease and sensorineural hearing loss should be minimally invasive, requiring local anesthesia, and induce a complete vestibular deficit while preserving hearing. Surgical procedures that involve the inner ear are considered the gold standard for Meniere's patients with persistent vertigo. These procedures are often less invasive than surgery and require little or no recovery time.
Temporal bone fractures
In one study, 77 patients with traumatic longitudinal temporal bone fractures were reexamined 12 to 20 years after the injury. The average follow-up period was 15 years. Although the progression of primary sensorineural deafness could not be demonstrated in this group, 38% had sensorineural hearing loss and 41 % had tinnitus. Twenty-four percent of patients had mild to moderate high-frequency hearing loss, while a further 4% had deafness in all frequencies.
Patients with head injuries usually present to emergency departments and trauma services. However, delayed referrals to specialists are not unusual, as they are often required to stabilize other co-morbidities. In addition, patients may be taking recreational drugs, which complicates initial assessment. However, the fracture path will follow the path of least resistance. The pneumatized portion of the bone is more likely to be involved in the fracture.
Upon a patient's presentation, an initial CT of the head and neck should be performed. The patient's temporal bone should be thoroughly evaluated, including a full audiometric assessment. A formal audiometric examination is needed if facial paralysis occurs. If immediate facial paralysis occurs, surgical exploration may be necessary. In contrast, delayed-onset or incomplete facial paralysis is typically treated conservatively with corticosteroid tapering.
Ototoxic exposure
Exposure to ototoxic chemicals may lead to sensorineural deafness. These ototoxic agents include medications for serious infections, heart disease, and cancer, as well as organic solvents. Noise and these ototoxic chemicals may interact to cause a synergistic effect on the cochlea hair cells, increasing the risk of occupational hearing loss. Exposure to both noise and ototoxins should be minimized.
Ototoxic agents can affect auditory function through various mechanisms, including ROS overproduction, inhibition of mitochondrial protein synthesis, and activation of apoptotic pathways. Ototoxic chemicals can also affect inner ear structures and neural pathways. Exposure to multiple chemicals can lead to varying degrees of sensorineural deafness. In addition to the exposure to chemicals, noise can lead to other health problems, including dementia and depression.
Since there is no standard way to monitor ototoxin exposure in individuals, the best course of action is to visit an audiologist. Audiologists are trained to assess and treat hearing disorders. If you suspect that you are suffering from ototoxicity, your doctor may recommend testing. Testing is often recommended for a range of reasons, including the severity of symptoms and the duration of exposure. Some medications can reduce symptoms and some people can even recover hearing after discontinuing exposure to an ototoxin.
Sources:
https://www.asha.org/public/hearing/Sensorineural-Hearing-Loss/
https://www.nidcd.nih.gov/health/noise-induced-hearing-loss
https://www.who.int/news-room/fact-sheets/detail/deafness-and-hearing-loss